PermanenteDocs Chat podcast on flu, COVID, and RSV vaccine safety and effectiveness updates with Sandra Fryhofer, MD, of the American Medical Association.
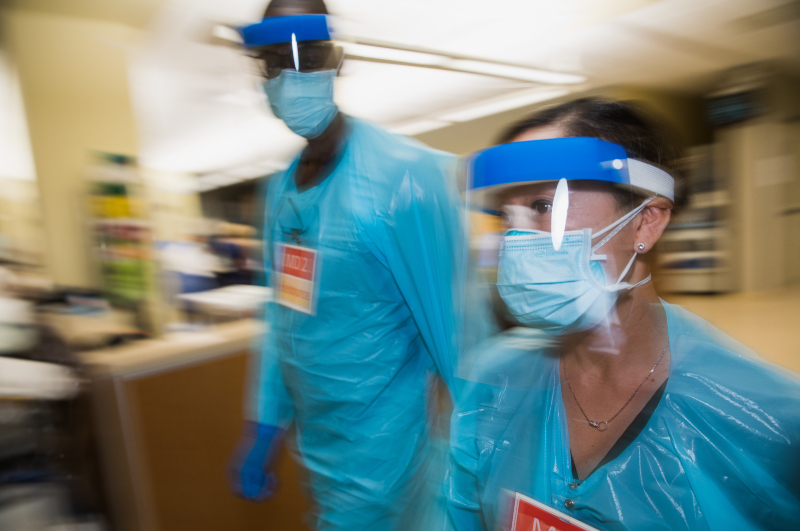
From the front lines: partners through pandemia
By Meighan W. Elder, MD
One short and very long year ago …

Whispered worries about Wuhan, initially dismissed, rapidly reaching a crescendo into panicked closures of borders, stores, and clinics. Fear-driven hoarding of hand sanitizer, toilet paper, and pasta. The first of many frantic reshufflings of our jobs and our lives. Laptops in closets. GlobalProtect and Doximity Dialer. Video without audio and audio without video. Screaming to be heard by the aged and ill-equipped.
The sudden absence of demand and then the beginning of the anxious calls about varied symptoms seeking testing, guidance, and certainty that didn’t exist. Virtual medicine in all the senses of the word “virtual.” Trading wisps of knowledge over Teams Chat — the beeping box in the corner of the screen the only anchor to colleagues and consults and collective determinations of what to say to our terrified patients (and ourselves). Working through lists of “caring calls” — wellness check-ins with older patients at greatest risk of coronavirus.
Digging out 20-year-old scrubs and donning patient-made masks or N95s buried in the back of desk drawers. Inching back out into a truly brave new world of sick clinics and well clinics, temperature checks and tents, PPE and PCR, home visits, and stripping down in the garage at night.
Leaving our children in front of screens and driving through the eerie quiet bearing our badges and feeling simultaneously essential and very much not. Listening to town halls with, hopefully, muted dread to the creep of COVID while cooking the hoarded pasta. Feeling grateful and proud to be part of the Colorado Permanente Medical Group and led by the strong voices of Margaret Ferguson, MD, MBA, Amy Duckro, DO, and Wendee Gozansky, MD.
These incredible women who stepped up to this unknowable task and taught us the terrible new lexicon of emergency operations. Command center end-of-day messages about PPE and the CDC and ICU bed numbers. Quarantine and home isolation and social distancing. Positivity rates and mobile morgues and hotel discounts for the front line.
Weeks turn to months
And then weeks turn into months consumed by spike proteins, ibuprofen avoidance, the 6-to-10 day window for COVID symptoms, aerosolizing procedures, swab shortages, Kaiser Permanente-made wipes, recycled masks, and anosmia. Surges in Seattle, Aspen, New York, London, Lombardy. Urban flight. Second-home spreaders. WFH (work from home) for the white collar. Grocery store workers as conscripted heroes. Reopening clinics, raw over-washed hands, resetting expectations. Financial fears, cancelled vacations, back-deck book club, endless home projects, lining up at the grocery store week after week. Zoom. All. The. Memes.
The brief reprieve of Summer and outdoor freedom fades into Fall with anti-maskers, mask shamers, presidential politics, federal failures, red-state/blue-state. Summer surges make way for college surges and the Winter to come laughs at them both. Forest fires burn and now the air is filled with smoke and virus. Asynchronous learning, blue-light glasses, sitting all day long.
Throughout this completely demented year the one constant … has been our physician assistants and physician partners.
Patients emailing for Tamiflu, hydroxychloroquine, albuterol, ivermectin, and remdesivir. (Learning how to say “no” and “it will be okay” in so many different, distracting ways.) No steroids but maybe steroids? Prone vent positioning but maybe avoid vents altogether? COVID anxiety briefly eclipsed by election anxiety. Collective breath held to get through the final weeks of this God-forsaken year, beaten down by daily doses of domestic terror lobbed by a tantrum-ing president and super-spreader holidays. We are all exhausted by the long haul of COVID. The quiet, overshadowed gift of the final days comes in the form of mRNA.
New year. Same old pandemic. The 2020 hangover wreaks treasonous mobs, ice storms, variants, and a vaccine rollout that unleashes aggressive-angry-anxious septuagenarians on a cowering COVID-battered health care system. There’s more, so much more. Collapsing kids and unspeakable violence and violation in the heart of our own town.
Glimmer of hope
A steady, calm drumbeat of science and sanity and societal resilience persists and gets louder. The 8 o’clock howls have faded but now we line up for jabs of this precious, fragile elixir that makes us feel simultaneously horrible, hopeful, and happy. Grandparents go back to grocery stores, hugs start to happen, and deferred disease management derails our days in a new kind of surge to normal.
Throughout this completely demented year the one constant (besides virtual everything) has been our physician assistants and physician partners. Providing answers to our often-unanswerable questions, picking us up when it was our turn to melt down, permitting us to vent, pivoting with all the constant change, and simply persisting. This particular world-changing crisis may not have allowed us to be healers so much as helpers — to our community, our patients, and each other. Caregivers in the fullest sense. As we cautiously climb out of this foxhole we have been in together and lean into hope and future-thinking, we look around at these steadfast partners and friends and feel thankful.
Meighan W. Elder, MD, is an internal medicine physician with the Colorado Permanente Medical Group. She practices in Boulder, Colo. This was originally published on National Doctors’ Day, which Dr. Elder likes to refer to as National “Partners” Day to include all care team members.

