Maria Ansari, MD, explores the concept of moral injury, how it impacts physicians' ability to practice medicine, and offers solutions.
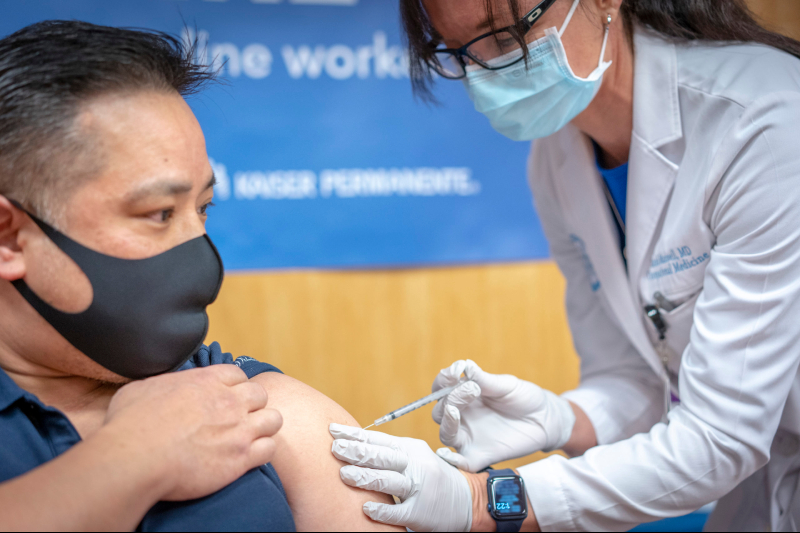
Turning COVID-19 vaccine hesitancy into vaccine confidence
5 ways to talk to patients about getting vaccinated when it’s their turn

As government officials and health systems work tirelessly to address the many logistical challenges of quickly vaccinating Americans against the coronavirus, we shouldn’t forget that these vaccines represent a glimmer of hope to end this pandemic.
The shaky start to COVID vaccine dissemination across states will soon be buoyed by increased supplies, including the new Johnson & Johnson vaccine and more on the horizon. In a few months, hopefully, we’ll be at a point where there will be a vaccine for anyone who wants it.
As we wait for that day to arrive, we as physicians must be prepared to sway the minds of people who may still be hesitant about getting the vaccine. Although more surveys find that the public is warming to the idea of the COVID vaccine — especially as a pathway to return to normalcy — nearly 40% of Americans still say they’re planning to sit on the sidelines and wait.
Here are 5 ways for physicians — a trusted source of health information for many people — to talk to patients about the COVID vaccine:
- Keep it simple. Use easy-to-understand language and don’t overcomplicate the process of getting a vaccine. Two of the currently available vaccines require 2 shots, but don’t dwell on details of refrigeration needs or differences in waiting periods. Stay focused on the vaccine as the protection they’ll need to return to activities they’ve missed during the pandemic. Johnson & Johnson’s new one-dose vaccine, which doesn’t require freezer storage, will also help keep explanations simple.
- Stay strong. Your clear, confident recommendation to vaccinate is important. Use statements rather than questions. For example, instead of asking if they want a vaccine, say, “When would you like me to schedule your vaccine appointment?” When answering questions about the vaccine, keep answers short and direct.
- Just the facts. Focus on the science and not the politics. Although the vaccines received emergency use authorization at an accelerated speed during the pandemic, each COVID-19 vaccine candidate met the Food and Drug Administration’s stringent safety and efficacy standards. During each phase of the clinical trials, data and safety monitoring boards followed the results closely to determine if the trial could continue. Still, recognize that the facts may not be everything to the patient.
- Don’t argue. Be careful to not fall into the trap of lecturing, debating, or arguing. Many people have long-standing opinions about vaccines. Hear them out, listen for what may be underlining concerns, and try to address what is truly feeding their hesitancy. Use personal examples to connect with their concerns: “I had those same feelings”; “My aunt felt the same way”; “I just saw a patient who wondered that too.”
- Be transparent. Like everything about this pandemic, there are many unanswered questions. We must be honest with our patients about what we don’t know about the vaccines so we can continue to be a trusted source for them. Still, emphasize that the benefits of protecting themselves and their loved ones outweigh any questions or uncertainty surrounding the vaccines.
Rebuilding trust in underserved communities
Traditionally underserved communities are among those hesitant to get the COVID vaccine. For many of these individuals, a higher threshold may need to be overcome before they will accept the vaccine, despite the promise of returning to everyday activities or seeing loved ones.
It’s important to acknowledge these real concerns. In the past, traditionally underserved communities have felt dismissed or marginalized. We should rebuild trust in the health system by listening and acknowledging the past.
Stress the benefits of helping their community along with protecting themselves.
When talking about the vaccine, point out that a broad range of people from all ethnicities and backgrounds were included in the clinical trials so that scientists could understand how the vaccines worked, as well as any side effects, in a variety of people. Help normalize the vaccine by identifying influencers who have gotten the vaccine or suggesting that they talk to a trusted community leader. Stress the benefits of helping their community along with protecting themselves.
Continuation of public safety measures
It will take some time for a large percentage of people to get vaccinated. Until then, we should continue to remind our patients of proven public-safety measures to slow the spread of the coronavirus: physical distancing, frequent hand-washing, limited group gatherings, restricted nonessential travel, and mask wearing. These practices should be continued even after getting the vaccine.
The COVID-19 pandemic has tested the doctor-patient relationship, forcing us to engage with our patients in different ways to help maintain their health while seeing them virtually. The vaccine holds the key to bringing some normalcy to that relationship and the promise of better health for our patients for many years to come.
Paul Thottingal, MD, is an infectious disease physician with Washington Permanente Medical Group and national infectious disease leader for Kaiser Permanente.


