Maria Ansari, MD, explores the concept of moral injury, how it impacts physicians' ability to practice medicine, and offers solutions.

The mental toll of providing care during a pandemic
Keeping watch for PTSD and other mental health issues for clinicians on front lines of COVID-19
By Michael J. Green
The Permanente Federation
The rising numbers of COVID-19 cases are staggering. However, when it comes to the mental and emotional toll inflicted by the novel coronavirus, some of the devastation cannot be quantified.
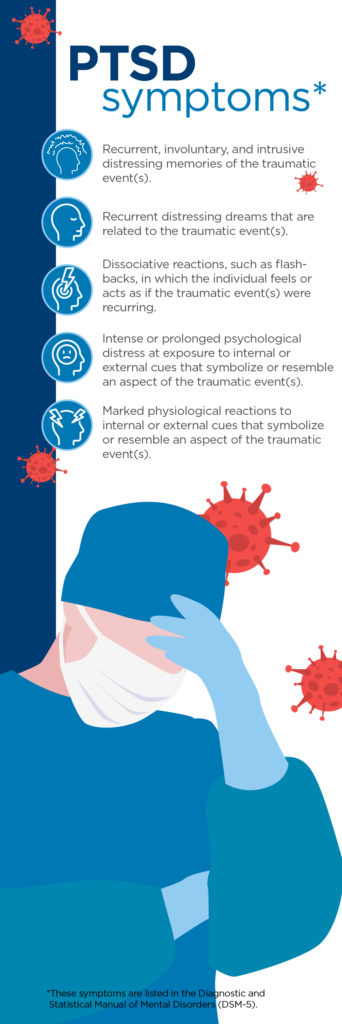
Over the last several months, the medical community has faced unprecedented challenges. As the pandemic plays out, the expectation is that a range of mental health issues could surface among health care workers. On the severe end of this spectrum are those who suffer from post-traumatic stress disorder or PTSD, a mental health condition that can occur among people who have experienced or witnessed traumatic events.

By the end of June, the Centers for Disease Control and Prevention reported over 2.5 million cases of COVID-19 in the United States and more than 126,000 deaths. The impact of these statistics has been deeply felt by those on the front lines.
“Health care professionals who care for people on the front lines of the pandemic can face a potent mix of traumatic experiences,” says Don Mordecai, MD, a psychiatrist with The Permanente Medical Group and Kaiser Permanente’s national leader for mental health and wellness. “PTSD is an extreme manifestation of how people may be affected by such a situation.”
Understanding PTSD
While many people associate PTSD with military veterans, a significant portion of Americans with symptoms are not. About 3.5% of adults in the United States suffer from PTSD, according to the American Psychiatric Association. Anyone who has been exposed to or threatened by death, serious injury, or sexual violence is at risk.
 Physicians and care teams may be exposed to a higher-than-average number of these factors through their regular work, Dr. Mordecai says. In the case of COVID-19, those caring for patients are witnessing firsthand unprecedented infection and mortality rates, without a cure.
Physicians and care teams may be exposed to a higher-than-average number of these factors through their regular work, Dr. Mordecai says. In the case of COVID-19, those caring for patients are witnessing firsthand unprecedented infection and mortality rates, without a cure.
“You have physicians and care team members being exposed over and over again to sick people all day,” says Dr. Mordecai. “It can take an emotional toll if you feel like you’re not able to help patients in the way you would want. At the same time, you need to be concerned for your own health and the health of your loved ones, which can add to the strain.”
Impact on specialties
While infectious disease experts, pulmonologists, and emergency room teams are often the ones called upon during this time, the impact of COVID-19 has been felt across many specialties. In some cases, physicians from other departments and non-frontline staff have been asked to step outside their familiar roles to help with the influx of patients.
“Certain specialties will be deeply impacted by witnessing the death of folks in isolation with a limited number of tools in their toolkit,” says Dawn Clark, MD, chief physician wellness officer and an obstetrician-gynecologist for the Southern California Permanente Medical Group (SCPMG). “Physicians may experience higher rates of PTSD as they are deployed into unfamiliar areas.”
Non-frontline staff show higher levels of distress than medical team members who are used to caring for patients with COVID-19, she adds.
More mental health considerations
The mental and emotional impact of COVID-19 on frontline workers may manifest itself differently from person to person depending on their experience — PTSD is just one of many possible outcomes.
“Most people experiencing traumatic events will not get PTSD, but they may well still have symptoms related to the trauma that they need to work through,” Dr. Mordecai says. “For a physician, it could be that they have trouble getting back to work after taking time off, or they might struggle with being in the ICU if that’s where a lot of the events happened.”
Early data out of China revealed that physicians and nurses who cared for COVID-19 patients showed higher rates of depression, anxiety, insomnia, and distress. Additionally, a study of the 2003 SARS epidemic detailed how hospital workers who were quarantined, worked in high-risk locations, or had friends or close relatives who contracted SARS were 2 to 3 times more likely to have elevated symptoms of post-traumatic stress compared with those not exposed to those elements.
Symptoms of moral injury
According to Dr. Mordecai, the concept of “moral injury” is another internal factor coming into play for medical professionals. Moral injury occurs when a traumatic event damages an individual’s conscience or values. Symptoms of moral injury may include grief, guilt, remorse, shame, outrage, or despair.
“Physicians and health care workers who essentially dedicated themselves to helping people can experience a moral injury when the world doesn’t let them do that,” says Dr. Mordecai. “With this virus, you don’t know how to treat it and a lot of people are dying.”
Physicians and care team members who cannot help as much as they want during the pandemic — for reasons such as not being trained in ICU medicine — may be at higher risk for feelings of guilt about not doing more, Dr. Mordecai says. This may also apply to members of the medical community who are unable to directly assist with COVID-19 spikes in certain regions because they are practicing medicine in a less impacted area.
A community of support
The Permanente Medical Groups (PMGs) have established a robust support system to address the mental health needs of Permanente physicians, care teams, and support staff. Kaiser Permanente programs in place prior to COVID-19, including employee assistance program and educational modules designed to help recognize mental illness, are being leveraged during the pandemic. One example is SCPMG’s “second victims” program, which reaches out to medical workers exposed to trauma through their work with patients.

“We’re seeking to promote all our internal and external benefits for mental health and emotional well-being, to help support those on the front lines of this pandemic,” Dr. Clark says.
To offer further support during COVID-19, Dr. Clark notes that SCPMG and other PMGs have participated in physician and leadership town hall meetings designed to educate leaders and the front line about top-of-mind physician concerns. These town halls have played an important role in guiding outreach and distributing information to medical staff.
The PMGs have helped frontline medical workers and those infected by COVID-19 to secure temporary shelter. Frontline workers have access to childcare resources and grants and extended paid sick leave benefits. Dr. Clark notes that medical groups have endeavored to identify and direct sources of PPE to internal supply chains, so that physicians have the resources they need to work safely.
“This gives our physicians more ways to protect colleagues and to see their efforts at work,” says Dr. Clark.
Sources of strength
With many resources available to address the mental health needs of physicians and care teams, ensuring that individuals feel empowered to seek out the help they need is of critical importance.
Dr. Clark says the destigmatization of needing and seeking emotional support is a priority. “Leader training for identifying needs, providing peer support, and making organizational resources more visible are all major focuses for helping our Permanente physicians and care staff right now.”
Within the medical community, there has been an outpouring of support among colleagues. Dr. Mordecai recalls stories of nurses flying across the country to help in COVID-19 hotspots, and he regularly sees notes from fellow physicians offering encouragement at his medical center in San Jose, Calif. Communities regularly show their appreciation for medical workers with signs, car parades, chanting, and other displays.
A strong support system of peers and neighbors, coupled with programs to address the mental health needs of clinicians, could ultimately prove pivotal for frontline workers in need of healing from the mental and emotional injuries inflicted by this pandemic.
“Feeling supported by your community can make all the difference in getting through a traumatic event,” Dr. Mordecai says. “We hope health care professionals saving lives on the front lines of the pandemic right now can look back and say, ‘This didn’t become PTSD or another serious condition because I wasn’t alone with it.’”


