Permanente Medical Groups led the U.S. in 2025 HEDIS rankings for preventive care, specialty care, chronic care, and behavioral health care.
10 ways physician-led health organizations provide exceptional breast cancer care (part 1)
This is the first of a two-part article highlighting 10 ways in which Kaiser Permanente and Permanente physicians offer exceptional breast cancer care. Read part 2 here.
A key advantage of being treated for breast cancer in a physician-led, coordinated, health care system such as Kaiser Permanente is the ability of Permanente physicians and clinical teams to care for patients over the entire continuum of care — from prevention to diagnosis to treatment or surgery to survivorship. Value-based care systems provide continuous, unfragmented care for breast cancer patients.
And because Permanente physicians have all of their patients’ information in Kaiser Permanente’s comprehensive electronic health records, they can seamlessly connect with each other, their patients, and the entire breast cancer care team, as well as designated family members and caregivers. Well-connected clinical teams support patients through all stages of breast cancer and carefully follow survivors in the critical years after a cure.
October is Breast Cancer Awareness Month. Learn 10 ways that Kaiser Permanente leverages its coordinated, integrated system — in partnership with physicians of the Permanente Medical Groups — to provide innovative, high-quality care for breast cancer patients.
1. Mammograms are key to early detection
Breast cancer is the second most-commonly diagnosed cancer among U.S. women, and an estimated 1 in 8 will develop invasive breast cancer at some point in their lifetimes.
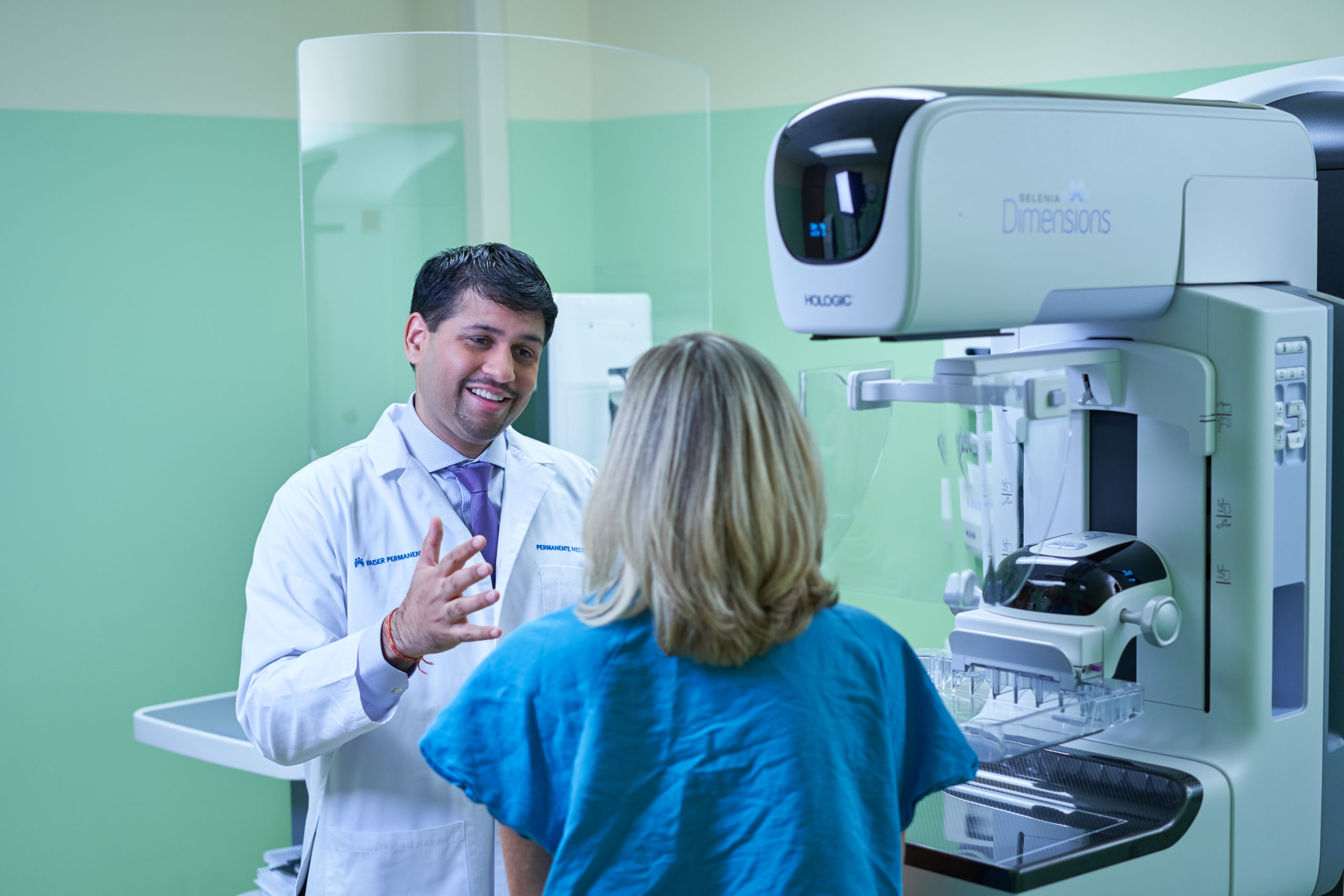
Mammograms are key to early breast cancer detection. With population-based screening, Kaiser Permanente has achieved screening rates better than 84%, compared with the national average of 73%. The integrated care organization is currently conducting 1 million mammograms every year nationwide.

Physician-led clinical care teams reach out to members who need breast cancer screening and make it easy for them to schedule their mammograms.
“Kaiser Permanente has consistently had some of the best breast cancer screening rates in the country. The COVID pandemic impacted mammogram rates not just in Kaiser Permanente, but nationwide,” said Nancy Gin, MD, executive vice president and chief quality officer for The Permanente Federation, the national organization for the more than 23,000 physicians who exclusively provide care to Kaiser Permanente members.
“Breast Cancer Awareness Month is a great opportunity to remind people to come in to get their screening done now because when breast cancers are caught early, at stage 1, the survival rate is nearly 100%.”
Related article: Kaiser Permanente members have lower mortality rates for breast and other cancers compared with national benchmarks
2. Genetic counseling helps patients understand risk
Breast cancer can be passed down from generation to generation; those with a first-degree relative (sister, mother, daughter) diagnosed with breast cancer have a higher risk of developing the disease. Genetic counseling provides a way for individuals to better understand their risk.

In Kaiser Permanente’s integrated system, people who believe they may have a higher breast cancer risk can use an online tool to help guide decisions about whether to be tested for the BRCA gene and other genetic mutations. Those who believe they may have a higher cancer risk are offered a consultation with a counselor in their local Kaiser Permanente genetics department, and if appropriate, referred for genetic testing and breast cancer screening.
“Catching breast cancer early begins with identifying members who are at higher risk of having an inherited predisposition to diseases like cancer and other disorders before they strike,” said Bethan Powell, MD, gynecologic oncologist, The Permanente Medical Group.
To alleviate anxiety about a possible diagnosis and provide full-service care, each higher-risk patient’s care team meets in advance to discuss their unique circumstances, then coordinates all needed services into a single visit. “A woman with a BRCA mutation, for example, will meet with a genetic counselor, a gynecologist, a breast surgeon, and — if she’s interested in prophylactic mastectomy — a plastic surgeon to discuss reconstruction,” Dr. Powell said. “She never has to leave the exam room.”
Related article: Kaiser Permanente member Faye Gordon enrolled in her region’s hereditary cancer program, which prepared her for a diagnosis of breast cancer at age 35.
3. Speedy mammogram results reduce worrying time
At Kaiser Permanente, mammography is made as easy as possible for patients by using the latest technology, delivering results rapidly, and enabling patients to communicate with radiologists about any troubling findings.

Even though patients benefit from screening mammography, many feel anxious about the process. Sometimes that anxiety is so strong that women don’t schedule their imaging exam to avoid the worry of waiting for the results.
At Mid-Atlantic Permanente Medical Group, screening mammography results are available to patients in less than an hour in most cases for tests scheduled during business hours on weekdays, while those who have mammograms on evenings or weekends will get their results the next business day.
“The results are read instantaneously by our fantastic group of board-certified radiologists,” said Helen Schneider, MD, radiologist with the Mid-Atlantic Permanente Medical Group. “And we eliminate the waiting. That very very stressful waiting.”
Related article: Mammogram results in less than one hour
4. Patients appreciate home recovery after mastectomy
In 2017, a team of Kaiser Permanente surgeons in Northern California launched an integrated program to offer mastectomy patients the opportunity to safely recover at home without overnight admission to the hospital. The program builds on Kaiser Permanente’s award-winning enhanced recovery after surgery (ERAS) program, which allows a carbohydrate drink before surgery (rather than the traditional fast), reduces opioids in favor of local anesthetics and acetaminophen, and gets patients walking soon after surgery.

“For a long time, it had been standard practice for mastectomy patients to be admitted to the hospital and discharged the next day,” said Brooke Vuong, MD, oncology surgeon with The Permanente Medical Group. “As surgeons, we would visit our patients the next morning, and they would usually be ready to go. We thought, what’s the added benefit of staying overnight?”
Care teams set expectations early, educate mastectomy patients and caregivers on the care and management of surgical drains at home, and follow up with patients after discharge by phone, video, or secure messaging. Telehealth provides mastectomy patients the welcome opportunity to receive most surgical follow-up care from the comfort of their own homes.
A 2019 study led by Dr. Vuong found that home recovery rates for Northern California mastectomy patients grew from 23% to 61% within 6 months of program launch, with no significant changes in emergency department visits, reoperations, or readmissions. Today 9 out of 10 of mastectomy patients treated at a hospital in Kaiser Permanente in Northern California recover at home after surgery.
Related article: There’s nothing like being at home
5. Surgeons deploy advanced breast surgery techniques
Kaiser Permanente surgeons deploy state-of-the-art surgical technologies for breast tumor removal and reconstruction, including with minimally invasive and robotic surgery.
For example, at Mid-Atlantic Permanente Medical Group, general surgeon Rahul Tevar, MD, (see video, below) uses radar localization to locate and remove breast tumors. Instead of placing a wire into the breast to help the surgeon find the tumor, the radiologist puts a reflector — akin to a small microchip — directly into the breast tumor, which helps the surgeon to precisely locate and remove the mass.
Jennifer Murphy, MD, plastic surgeon and chief of Plastic Surgery at Northwest Permanente, pioneered the use of fat-grafting techniques for total breast reconstruction, providing an alternative for women seeking to avoid breast implants or the more painful “flap” procedure.
“While we had seen success in this small-scale fat grafting, no one had recreated an entire breast with this technique,” Dr. Murphy said. “Total breast reconstruction helps women to feel ‘normal’ after having had a mastectomy. I find joy in helping them conquer their disease.”
Related article: Fat-grafting use in innovative breast reconstruction
Note: To learn more about how Permanente physicians provide exceptional breast care, view part 2.


