Maria Ansari, MD, explores the concept of moral injury, how it impacts physicians' ability to practice medicine, and offers solutions.
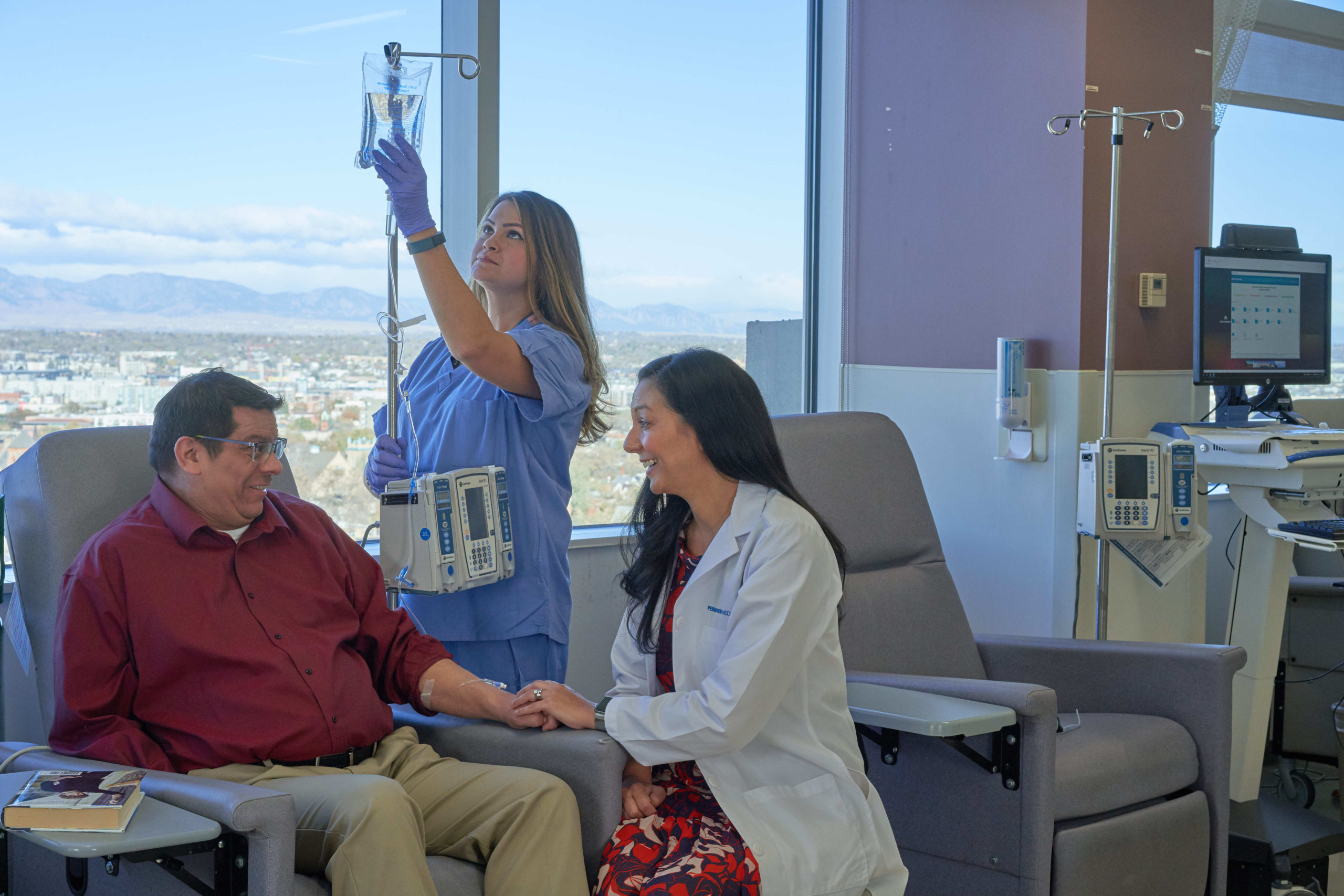
Surviving, and thriving, after cancer
Cancer patients in Kaiser Permanente’s integrated health care system are living longer and better

When Robert Binkley of Yorba Linda, Calif., was diagnosed in 2006 at age 57 with chronic lymphocytic leukemia — an incurable cancer of the white blood cells in his bone marrow — his Permanente physicians told him that he could expect to live about 10 years.
Eight years later, at age 65, he joined a clinical trial for a targeted, “precision medicine” cancer treatment, and he has been in remission ever since.
“It was a great decision for me to go on this clinical trial,” says Binkley, now 72. “I try to keep a positive attitude, and I wasn’t about to let this illness hold me captive.”
Binkley is not alone. Due to better screening, early detection, and innovative new treatment options, more and more patients are not only surviving cancer diagnoses, but also living longer and living well. As of January 2019, the National Cancer Institute estimated that there were nearly 17 million cancer survivors in the United States, about 5% of the population. That number is expected to increase more than 30% to 22.2 million by 2030.
Screening and prevention save lives
A Kaiser Permanente study published in the American Journal of Managed Care found that our members in Southern California with 8 common cancers (breast, prostate, lung, colon, melanoma, uterine, kidney, and bladder) had better survival rates over a 5-year period than those with other types of health insurance coverage. Importantly, the study of 165,000 people found that Black cancer patients diagnosed at non-Kaiser Permanente hospitals had an astonishing 14% higher risk of death and Latino patients had a 23% higher risk of death compared with those who received care from us.
More people are surviving cancer in our health care system in part because they are better screened for preventable cancers — especially breast, colon, and cervix — across our large, diverse populations. For example, Kaiser Permanente members in Northern California were 52% less likely to die from colorectal cancer after we launched a comprehensive, organized screening program.
Surviving with high quality-of-life
Cancer patients receiving their care at Kaiser Permanente are followed carefully and supported throughout all stages of cancer.
Because we have all of our members’ information in our electronic health record, we can connect their cancer care with any other medical concerns they may have. Health issues such as diabetes, heart disease, and obesity do not go away when cancer is diagnosed and treated. Familiar, trusted physicians and care teams, who have overseen care for patients all along, understand and manage all of their cancer patients’ health concerns during treatment and beyond.
I try to keep a positive attitude, and I wasn’t about to let this illness hold me captive.
— Robert Binkley, a Kaiser Permanente member
Research has shown that up to three-quarters of cancers in the United States are preventable. With guidance from their doctors and the support of nutritionists and lifestyle coaches, Kaiser Permanente members are learning to incorporate healthy-living strategies that stop cancers from starting in the first place, while cancer patients are seeking to build upon their treatment success to prevent future cancers from occurring. By smoking less, eating better, exercising more, and reducing stress, cancer survivors are often living better than they did before being diagnosed and treated.
“I bike ride, I walk, I play golf, I travel, I work in the yard, I do home remodel projects. I constantly try to stay healthy in any way that I can,” Binkley says. “Sometimes I do things that are maybe too high-risk for my wife and my doctor … But all of this activity helps me keep the right mental frame of mind, and I think the mental frame of mind helps us a lot in battling cancer.”
Paying it forward
At Kaiser Permanente, research and clinical practice are integrated to create a virtuous cycle of continuous improvement. Physicians draw upon their medical experience to propose cancer research; the results of those studies are then taken by physicians and clinicians and applied to create new, evidence-based approaches that improve cancer care, treatment, and outcomes.
At the same time, participating in clinical trials and survivorship research creates community and empowers cancer survivors with opportunities to pay it forward.
“I hope people aren’t scared away by the term ‘clinical trial,’” Binkley says. “They’re so well researched and are not offered until they’ve shown themselves to be of benefit to patients. I think it’s important that people like myself get involved in these things, not only for our own benefit, but for the benefit of others who come after us.”
Nancy Gin, MD, FACP, is executive vice president of quality and chief quality officer for The Permanente Federation.


