Stephen Parodi, MD, examines the growing gap between the power of vaccines, public trust, and preventable diseases
Kaiser Permanente Research: Relevant to Today’s Policy Challenges

Value-based insurance design (VBID) is a buzzword getting attention from policymakers and stakeholders in search of ways to improve consumer incentives and purchase coverage with better value. Mary Reed, PhD, of Kaiser Permanente’s Division of Research in Northern California, and her colleagues have been steadily publishing reports on consumers’ utilization response to changes in benefit design and new access options such as email and phone calls with physicians.
Reed’s research is based on the experience of real Kaiser Permanente members. The size and diversity of that membership makes the research even more relevant. She was recently in Washington, DC, to describe her team’s latest findings on the effects of benefit design on medication adherence among consumers with chronic conditions.
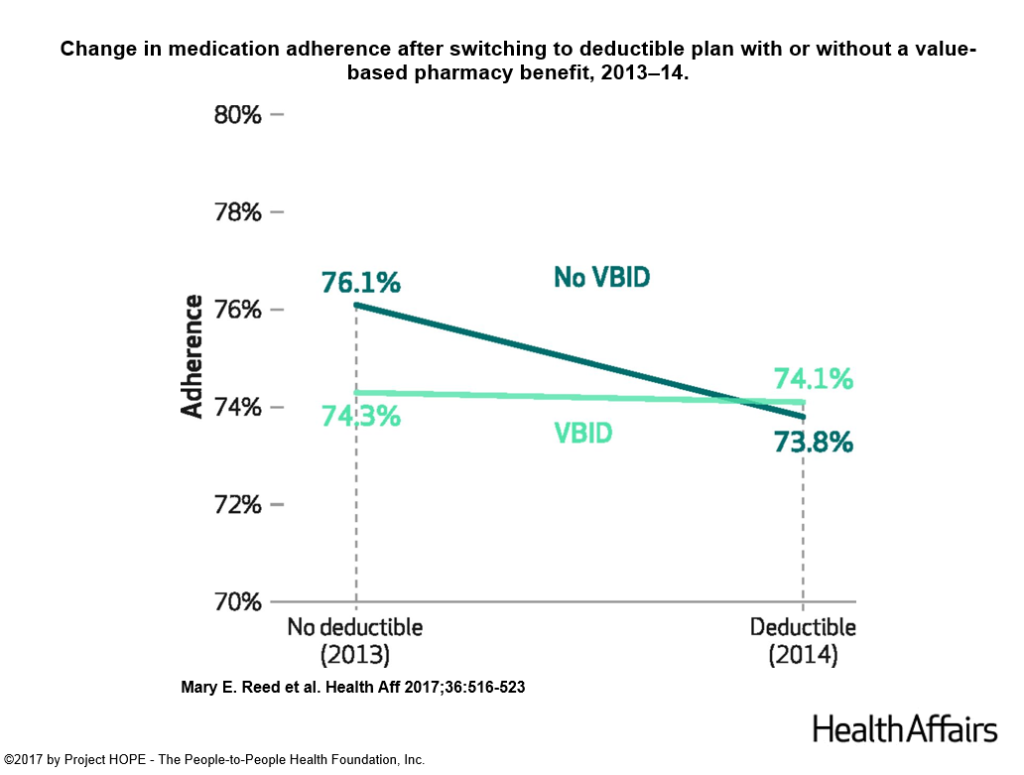
Comparing Kaiser Permanente members enrolled in plans without cost-sharing for medications for chronic conditions (the VBID group) with members who faced deductibles for these medications, Reed found that the members facing deductibles had lower rates of medication adherence.
When she and her colleagues dug deeper into the data, they discovered that members living in lower income neighborhoods had lower rates of using medication as prescribed even when enrolled in the $0 co-pay VBID plan. The VBID design alone does not appear to be enough to help these enrollees improve their medication adherence, and suggests other barriers must be addressed for more economically disadvantaged consumers.
You can see Reed in action here.